Facing Our Antibiotic Dilemma
Jordan Reinbold
INTRODUCTION
When you get ill, hurt,
need medical advice or surgery, you go to a hospital. A person doesn’t arrive
at the hospital thinking their visit may kill them. In reality, hospital
infections kill more than five times the people than AIDS does in the United
States. They account for more than 100,000 deaths a year (McCAUGHEY,
2006). This paper will address a few of the most dangerous antibiotic-resistant
and antibiotic-caused bacterial infections, examine a specific study, and
discuss possible solutions. The three “bugs” that will be discussed are methicillin-resistant staphylococcus aureus (MRSA), clostridium
difficile, and vancomycin-resistant enterococcus faecium (VRE). After these three bacteria are discussed, a
specific case will be reviewed. Following the case study, a transcript of an
interview with Julie Ternes, an RN, is included.
MRSA
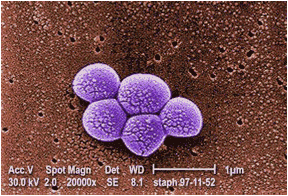
The
above image of a microscopic view of MRSA was taken from a webmd.com article
entitled “A closer look at MRSA”. MRSA was first discovered at a hospital in
1961 in the United Kingdom. The whole history, however, would include the
discovery and misuse of antibiotics that led to the resistance itself which
can be read about in Jessica Kopp's discussion of the history of antibiotic resistance. Since the 1960’s, MRSA has
continued to grow as a problem and now is considered one of the most common
hospital born infections (historyofmrsa.com).
MRSA is considered a superbug, meaning it has a resistance to multiple types of antibiotics. In many cases, the symptoms of MRSA are manageable if found right away. Common systems of MRSA are skin and soft tissue trouble; these symptoms include cellulitis, impetigo, boils, and abscesses (historyofmrsa.com). It is spread through direct contact, such as the brush of a sleeve or using bed railings that are contaminated. The problem with treating MRSA is that it is resistant to nearly all common forms of widely used antibiotics. The superbug is also growing increasingly resistant to the few drugs that effectively kill it. In this country alone, between the years of 1976-2003, the cases of MRSA in hospitals increased 32 fold (McCAUGHEY, 2006).
Luckily, there are still a few antibiotics that work;
however, most of them are available only intravenously. While most hospital
acquired cases are diagnosed in the hospital, receiving intravenous drugs
usually doesn’t pose much of a problem. In these settings the necessary equipment
for IV treatment is readily available; however, it does prolong the hospital
stay and make the hospital bill even more costly. Despite the danger MRSA poses,
recent trends show that there is a decrease in ICU’s around the nation.
According to a CDC article, S. aureus and MRSA Surveillance Summary, central line-associated
bloodstream infections reported from hundreds of different intensive care units
have decreased 50-70% between 2001 and 2007.
VRE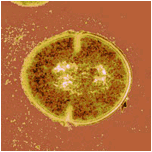
(image
from forbes.com)
Vancomycin-resistant enterococcus faecium (VRE), shown above, is another antibiotic-resistant
bug that started to get attention in the 1980’s. It is resistant to an
alternate family of antibiotics in relation to MRSA. Like most all resistant
bacteria, VRE can be fatal if it is allowed to progress too far (VRE:
Information for the Public). One of the scary aspects of VRE is that it has an ability to easily
pass on its genetic resistance to other bacteria. Scientists are still
investigating the specific mechanisms VRE uses to easily spread its resistance.
Why does this pose such a serious problem to investigate? In 2007, there were seven
cases of VRSA (vancomycin-resistant) staphylococcus aureus). Studies showed that at least
one of these cases was caused by the transfer of resistant genes from VRE to form
VRSA . Vancomycin is a
useful last resort treatment for MRSA, and if VRE continues to contribute its
resistance, we may slip farther behind in the battle we are fighting with MRSA.
C. DIFFICLE Clostridium difficile is another hospital acquired
infection of concern. According to the Office of National Statistics (ONS),
cited by BBC news, deaths involving C. difficile rose by 62% from 2004-2005.
This number seems strikingly large, and the ONS admits that the fact that there
is increasingly greater awareness surrounding hospital infections, more
hospitals and doctors may have been inclined to report C. difficile as a
possible contribution to death. The number which might be slightly inflated
still represents a problem.
C.
Difficile is slightly different than MRSA, as it lives in the intestinal tract
of humans. About 3% of adults and 66% of infants carry C. Difficile without any
problems (BBC, 2007). The problem arises when the normal flora of the stomach (healthy
bacteria that live in the stomach) is disrupted. When in the hospital for an
extended stay, it is very likely you will be receiving antibiotics while you
are there, which can inadvertently kill some of the healthy bacteria in your
stomach. This allows C. difficile to start taking over the now vacant space. C. difficle is very strong in its spore
form, making it difficult to kill with basic methods of alcohol based hand
washing. The spore can survive on surfaces for long periods of time waiting to
be picked up and ingested. A Look into Specific Case (Sorberg,
Farra, Ransjo, Gardlund, Rylander, Settergren, Kalin, Kronvall, 2003) The
following is a case study that helps to illustrate how antibiotic resistance
grows over time. The case is a 12-year study that was conducted at Karolinska Hospital (university
hospital that utilizes six intensive care units). Only the non-pediatric ICU’s
were used in this study. The
hospital measured the resistance of E. coli in relation to several different
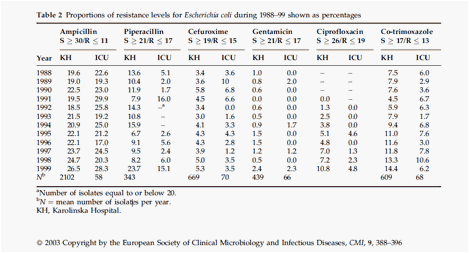
antibiotics. The results are shown on the table below.
The
above table reviews the results of the 12-year E. coli study. E. coli,
intestinal tract bacterium, grew in resistance to several types of antibiotics.
This unfortunate trend is common among most bacteria with high exposure to
antibiotics.
PREVENTION
On
the positive side, there are things that can be done to help control the spread
of antibiotic resistance. One study found how monitoring the way antibiotics
are prescribed can have an effect on growing resistance. A study published in an issue
of Infection Control and Hospital Epidemiology described three ways of
prescribing antibiotics:
- Preventative-
administered before or during
surgery
- Empiric-
administered before the doctor is positive of the bacterium
- Targeted- administered once a certain diagnosis has been made.
The study showed how
hospitals that specifically monitored and put regulations on empiric
prescribing had lower rates of antibiotic resistance. (Indiana University, 2006).
Other methods, such as proper hand washing (Weinstein, 2009) and a better
public awareness (Tomasz, 1994) can also be effective in reducing the number of
antibiotic resistant cases.
INTERVIEW
Along with the literature review, an
interview was conducted to provide additional information about what current
educators are doing to correct the problem as we go forward. The following
interview was conducted through e-mail with Julie Ternes. Ternes is currently an
RN, BSN, and has been working as such for 8 Years. Her experience has been on
an in-patient surgical floor where patients are taken care of after surgery
until discharged. She is currently in her second year in the Doctorate of
Nursing Practice program at North Dakota State University. She is set to
graduate in December 2011. The interview is shown below in its entirety.
Questions:
- Are you aware of the growing problem of antibiotic resistance?
As an in-patient nurse I took care of numerous patients that had some form of resistance to antibiotics. The majority of the resistance appeared to be MRSA, VRE, and C-diff. Not only is it a hazardous risk for the patient to be resistant, but also to the staff that are taking care of these patients. As a RN, we work in close contact with the patients making transmission relatively effortless. Current policies are now in effect making transmission less accessible with the use of proper isolation precautions (gowning, gloving, hand sanitation). Another view is looking at the productivity lost by having to use these precautions—it is timely and also takes care away from other patients.
- Do you
feel that, as a student that will soon be able to hand out prescriptions, you
will be prepared to take on the problem?
First off, I don’t consider myself one that will “hand out” prescriptions; rather, I will be prescribing them when appropriate. Thurs far, I have witnessed providers give antibiotics for some common complaints of sinus congestions in which the patient thinks he/she has an infection when in reality it is usually part of the viral process. Sinus infection doesn’t typically set in until usually week 4-6; however, most individuals do not want to wait that long to start feeling better, so they go to the local provider with the mindset that they will get an antibiotic and start feeling better sooner rather than later. As a student I am well aware that patients come to the clinic to get something to make them feel better; however, antibiotics are not always the right thing. For example, if I was the NP seeing a patient with complaints of sinus complaints for 3 days, I may recommend them taking a mucolytic to help break up the secretions to help open the sinus cavities—by doing this you are getting rid of the secretions decreasing the chance for them to set in the sinus cavity and turn into a bacteria. Yes, I feel I will be prepared to “prescribe” appropriate prescriptions.
- Has
your graduate education addressed the problem and/or solutions?
In my program, this topic has been brought up numerous times. As students we witness different practice done by different providers and usually share them in class. As NP students we have our nursing background to help us treat the entire patient; by treating the entire patient of body, mind, spirit, we strive to do what is best for them….antibiotics are not always what’s best for them.
- What is your plan for prescribing antibiotics in the future?
As explained above, I plan to use my professional judgment as to when antibiotic therapy will be appropriate. For non-life threatening situations I plan to obtain culture before prescribing antibiotics to be able to treat with the appropriate antibiotic therapy. Also, I plan to educate patients that although antibiotics may be the “quick fix” they are not the best treatment plan for them. I plan to have patients get upset with me and seek other providers; however, I plan to approach the situation with the goal to do what is best for them, not what they want me to do for them. I plan to have open communication that allows for educational opportunities for the patients to understand how and when antibiotics should take place.
- Do you feel as though your mindset about prescribing antibiotics is a product of your education from NDSU, or your personal research?
I can’t say it's one or the other. I think it's a combination of the two. I had previous knowledge regarding the use of antibiotics; however, the knowledge from the graduate classes along with my instructors and preceptors have led me to my current aspirations to be able to prescribe correctly, efficiently, and most of all, safely.
CONCLUSION
In summary, the general public should
be aware of the antibiotic resistance problem our universe is facing. MRSA,
VRE, and C. Difficile are some of the most common and dangerous bugs that are
encountered in the hospital setting and can be potentially fatal. Through
better efforts in sanitation, further research, and better prescribing methods,
we can begin to remedy the situation.
References
Chang,
L. (2010, February 25). Mrsa slideshow: a closer look at mrsa. Retrieved from http://www.webmd.com/skin-problems-and-treatments/slideshow-closer-look-at-mrsa?ecd=ppc_google_whatismrsa_Skin_MRSA-Overview++Facts++EducationandCauses_search&gclid=COmR54LKgKUCFY4B5wodmiYb8Q
Farra, A., Ransjö, U., Gårdlund, B., Settergren, B., & Kalin, M. (2003). Different trends in antibiotic resistance rates at a universityteaching hospital. Clinical Microbiology and Infection, 9(5). Retrieved from Academic Search Premier database.
Herper, M. (2006, March 1). The most dangerous bacteria . Retrieved from http://www.forbes.com/2006/03/01/antibiotics-pfizer-cubist-cx_mh_0301badbugs.html
Indiana University (2006, October 12). Controlling Antibiotics And Antibiotic Resistance In Hospitals. ScienceDaily. Retrieved November 1, 2010, from http://www.sciencedaily.com/releases/2006/10/061010022439.htm
Mcaughey, B. (n.d.). To Catch a Deadly Germ - New York Times. The New York Times - Breaking News, World News & Multimedia. Retrieved November 24, 2010, from http://www.nytimes.com/2006/11/14/opinion/14mccaughey.html?_r=1&oref=slogin
Mcaughey, B. (2007, February 7). Hospital bug deaths on the rise. BBC News. Retrieved November 22, 2010, from http:/http://news.bbc.co.uk/2/hi/health/6385323.stm
S. aureus and mrsa surveillance summary. (2010, August 3). Retrieved from http://www.cdc.gov/mrsa/library/MRSA-Surveillance-Summary.html
The History Of MRSA and Why it Developed. (n.d.). History of MRSA. Retrieved November 24, 2010, from http://historyofmrsa.com
Tomasz, A. (1994). Multiple-antibiotic-resistant pathogenic bacteria -- a report on the rockefeller university workshop.The New England Journal of Medicine, 330. Retrieved from http://www.nejm.org/doi/full/10.1056/NEJM199404283301725
Q&A: Clostridium difficile. (2007, August 19). BBC News. Retrieved November 24, 2010, from http://news.bbc.co.uk/2/hi/health/6252151.stm
VRE: Information for the Public FAQ | CDC Infection Control in Healthcare. (n.d.). Centers for Disease Control and Prevention. Retrieved November 24, 2010, from http://www.cdc.gov/ncidod/dhqp/ar_VRE_publicFAQ.html
Vancomycin-Resistant Enterococci (VRE). (n.d.). MedicineNet. Retrieved November 21, 2010, from http://www.medicinenet.com/vancomycin-resistant_enterococci_vre/article.htm
Weinstein, R. (2009). Controlling antimicrobial resistance in hospitals: infection control and use of antibiotics. Retrieved from http://www.cdc.gov/ncidod/eid/vol7no2/weinstein.htm
If you would like to see previous comments or leave comments about this website, click on the comment button below.
